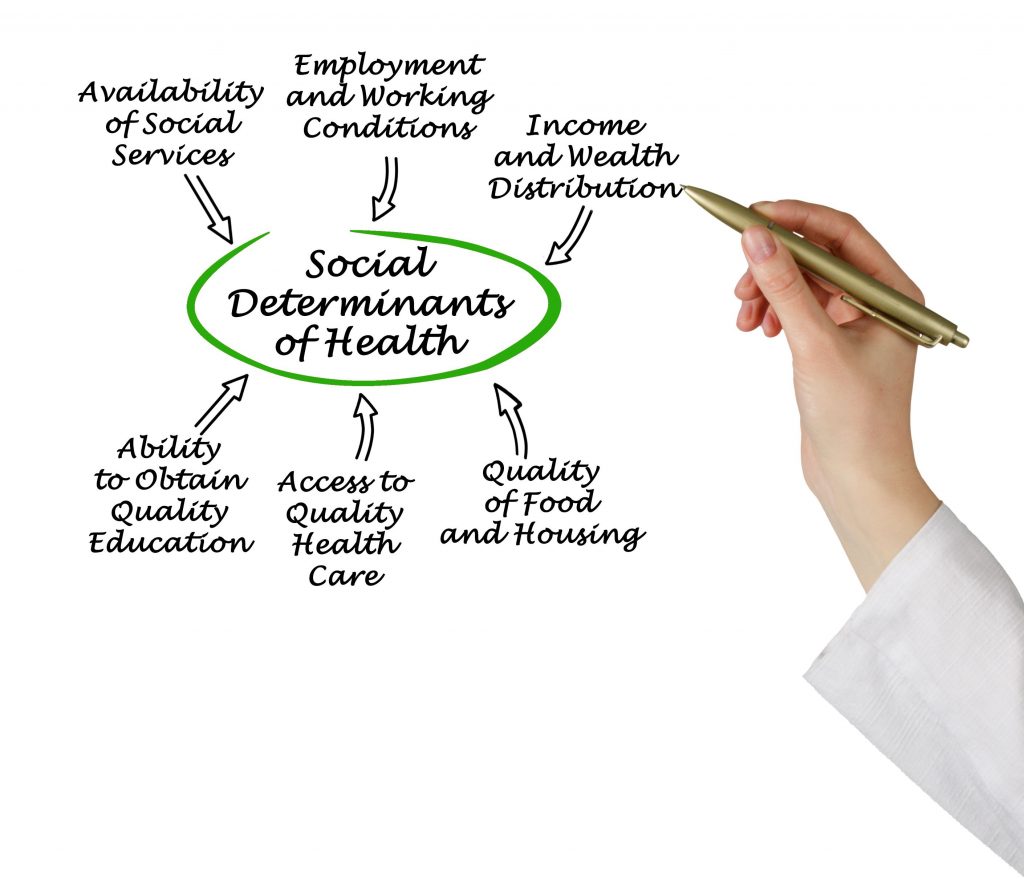
As the shift to value-based care takes shape, the role social determinants of health (SDoH) should play in creating personalized care plans and precision medicine initiatives has become clearer from both a business and care perspective.
The World Health Organization defines social determinants of health as “the conditions in which people are born, grow, work, live, and age.” Incorporating these factors into a patient’s health management has been linked, according to the Robert Wood Johnson Foundation, to better patient outcomes and decreased costs.
As things currently stand, SDoH is not being worked into the clinical workflow universally. Data currently collected by medical professionals regarding SDoH is largely unstructured, and whether or not a provider is incorporating it into electronic health records (EHRs) is still unpredictable. According to a study from Deloitte, less than one-third of hospitals are integrating social needs into the EHR for most of their target population.
Bringing that data into EHRs is vital as it could potentially increase access to SDoH data while also standardizing it, enabling aggregation across a wider range of systems. Doing so will also require the development of medical terminology codes that reflect SDoH data.
Applying SDoH to the EHR
As providers, insurance companies and government agencies look for the best ways to incorporate SDoH data, EHR vendors also have to determine the requirements necessary for this type of data to be functional and interoperable. According to a blog post from EHR vendor Cerner, the following capabilities are necessary for EHRs to help providers make the most of this new data.
- Make SDoH data visible at the point of care
- Develop social care plans that are integrated with clinical care plans
- Assign each task to appropriate team members
- Link resources aimed at addressing needs expressed in the care plan automatically
- Provide patients with resources that connect them with social services
The U.S. Core Data for Interoperability initiative has identified many social factors under its emerging set of data classes that are under consideration for being added to the list of data required to be collected in FHIR or C-CDA format and shared through fully interoperable EHRs. They include areas such as level of education, financial resource strain, social connection/support, exposure to violence, employment status, stress assessments, military history and physical activity levels.
It also lists a category broadly named social, psychological and behavioral data, meant to provide information regarding “…conditions in the places where people live, work, learn and play that can affect health risk and outcomes.”
But collecting this data and integrating it borders on uncharted territory. A study published in the Journal of the American Board of Family Medicine which examined the effect of aggregating and presenting SDoH data in an accessible way used the EHR system of the Oregon Community Health Information Network (OCHIN). It included ideal patient demographics for a study of its kind and tools designed to help social workers identify and address SDoH concerns as well as align workflows with the clinical referral process.
In the end, the study concluded that “to attain these potential benefits, health care organizations need guidance on how to facilitate systematic SDH screening in primary care settings using EHR-based tools.” There’s just one problem with that. There is no guidance for doing so to date.
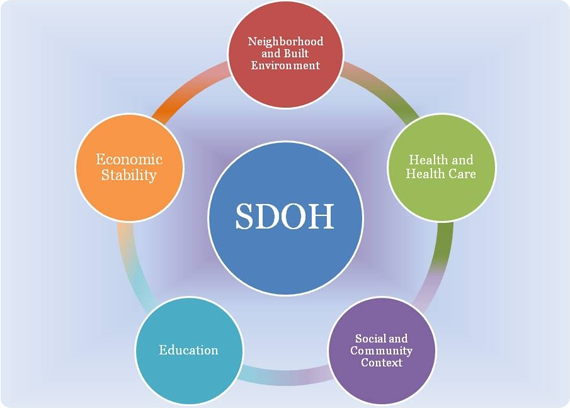
Knowing how to categorize the data may help. This is the goal of the Healthy People 2020 initiative from the Office of Disease Prevention and Health Promotion, which focuses on what they refer to as a “place based” framework for organizing key areas of SDoH data. That includes five determinant categories, outlined in the graphic below.
SDoH Impact on Value-Based Care
According to the Centers for Disease Control, social determinants of health have a bigger influence on health outcomes than the delivery of patient care. Value-based care models are based on insurers paying providers for health outcomes rather than services provided, therefore, looking at SDoH data is becomingly increasingly important.
Adoption of SDoH data is growing amongst payers, with 80% of them integrating SDoH into their member programs, according to a study from Change Healthcare and the Healthcare Executive Group. Beyond improved outcomes, payers are encouraging the widespread adoption of SDoH data due to its impact on costs.
By examining SDoH data, providers can make predictive models capable of more accurately identifying patients with a higher risk of readmission or identify which patients need in-home visits versus a simple follow-up phone call following a procedure.
In general, outcomes that SDoH data can help payers monitor include mortality, morbidity, life expectancy, expenditures, health status and limitations, according to a report from LexisNexis. The report from the risk management service outlines data attributes they’ve created from public and proprietary records and are testing.
For example, the report states that “Validated socioeconomic attributes correlate to health outcomes including cost, hospitalizations, readmissions, ER visits, medication adherence, motivation and stress.” It even goes as far as outlining “correlating derogatory attributes” such as arrests, liens, bankruptcies, evictions, neighborhood crime rates, unpaid debt and loan applications.
Tailoring Care and Increasing Awareness
Across the board, from providers to payers, social service agencies and data analytics vendors, there is a belief that SDoH data can provide a more holistic view of the patient’s life and improve risk assessment predictions that will tailor care to the individual more accurately.
An article from Healthcare IT News highlights an example from health insurer Humana honing in on a specific social issue and in doing so, drastically reducing costs.
By examining the issue of food insecurity specifically, the Louisville-based insurer found that those dealing with food insecurity are 50% more likely to be diabetic, 60% more likely to suffer heart failure and 14% more likely to be living with hypertension. The company’s research shows that catching these conditions in an early state can reduce spending by 34%.
The company found that by screening members at risk of food insecurity and offering SNAP benefits and emergency food boxes to those who qualified, they were able to decrease the amount of days those patients were mentally or physically unwell by half.
“I once sat through an hour lecture on why children fail to thrive, and every possible differential diagnosis was discussed except the possibility that maybe they didn’t have enough food,” pediatrician Sandra Hoyt Stenmark said in an interview with the Association of American Medical Colleges.
Stenmark helped lead Kaiser Permanente Colorado’s initiative to collect food insecurity data and integrate it into their EHR, approving outreach from a nonprofit organization on the patient’s behalf. The case first must go to a community specialist with KCPO, who then notifies the nonprofit, meaning fully interoperable systems must be in place to ensure that the data flows. Stenmark thinks that buying into the importance of SDoH data at an earlier stage for physicians will also help.
“I think medical schools would really benefit from having some emphasis on the medical role in meeting patients’ social and nonmedical needs,” she said.