The waiting is the hardest part.
“Anyone who’s ever been in the hospital knows that when you’re sick and waiting it’s the worst experience ever because it’s amplified. Every minute you’re in pain or not feeling better, it feels like an hour, a day, a week.”
So said Dr. Peter Chang, an assistant professor at USF Health’s Morsani College of Medicine at the University of South Florida. Chang, who also is the vice president of Care Transitions at Tampa General Hospital (TGH), wants to decrease that wait time.
A 9,000 square-foot, artificial intelligence-based care coordination center, scheduled to open at TGH next year, promises to address wait-time issues and a whole lot more.
Created by General Electric and most often referred to as Command Centers, the concept is analogous to an air traffic control tower, where events can be observed and coordinated as they happen.
The technology “allows us to monitor all of our patients in our hospital in real-time,” said John Couris, CEO of Tampa General. According to Couris, a variety of coordinating elements will be overseen at TGH’s Command Center, including the transfer center, staffing office, environmental services and patient transport.
The Command Center’s purpose is to create a seamless flow of all elements of patient care. All of the hospital’s departments will be represented in the center, which will help departments collaborate and anticipate where people need to be and when they need to be there. This will create an optimal patient experience and “support our nurses, physicians and our allied health professionals to the best of our ability.”
“This is going to be a transformational change for us,” Couris said.
World Cup Origins
The command center’s origins go back to the 2014 World Cup.
As reported in The Guardian, host city Rio de Janeiro wanted to coordinate and improve the effectiveness and efficiency of its civic services in preparation for the huge crowds of international soccer fans arriving.
The city enlisted IBM Brazil, which created a system that brought 30 city departments into one room to track the municipality’s needs in real-time.
Jeff Terry observed the Command Center when he visited Rio as part of a group of analytics experts the city brought in to discuss how healthcare could be handled during the World Cup.
Terry, CEO of Command Centers for GE Healthcare, thought they would be an excellent fit for hospitals. Rio passed on the idea, but Terry believed it was just a matter of finding the right recipient.
”When we shared the idea with Johns Hopkins , there was sort of a eureka moment where we all said, ‘That’s it! Let’s do it,’” Terry said.
“What is the command center? It’s a new department, a team of people working around the clock to help care teams,” Terry said. “What’s a new department? A new group of people, and some are existing staff with redefined jobs.”
Employees in the new department aren’t ordinary staff members: they are subject matter experts with an intimate knowledge of how solutions will plug into workflows and issues healthcare professionals need addressed.
“We call it problem-backed design,” Terry said. “You spend weeks elbow-to-elbow with caregivers, really drilling into what the problems are: What would help you? What don’t you know? What’s your frustration? What do patients get frustrated about?”
Designers spend weeks interviewing staff from all areas of the facility to discover as many problem areas as possible.
“It’s a hundred, or a thousand, very specific problems that the command centers go after,” Terry said.
“These are teams of people coming from the front lines,” TGH’s Couris added. “These are bedside nurses and therapists and physicians helping to figure out how to do the work that we’re doing today differently to drive better quality, better safety, service, overall performance — what we’re calling world class performance.”
New Title, New Organization
Before the implementation of the command center at Toronto’s Humber River Hospital, Jane Casey’s title was Program Director for Emergencies. Now she’s known as the Command Centre director, but much more than her title has changed.
“I’m doing the same job, but before I was blindly doing it, trying to figure out where people were,” Casey said. “Now, I have the information right in front of me. The team is all together. Before we were sort of on a treadmill working very hard without the right information. We were not consistent on the actions we took, and staff were scattered throughout this building.”
Scattered staff, information and instructions have historically been a problem for hospitals.
“You could be a patient in our hospital and you could have five or six different consults at any given time,” said Couris. “You could have a GI (gastrointestinal) doctor, a cardiologist, a neurologist, an infectious disease physician, primary care doctor and a urologist. You have six different doctors trying to figure out what’s wrong with you.“
The problem with this, Couris said, is that “doctors are notoriously bad at communicating with each other. They’re great clinicians, but you need those physicians actually talking to each other. Imagine having a care coordination center that manages all of that. Imagine if all of your specialists were communicating with each other efficiently and effectively, and they were doing it in a timely way.”
Healthcare Meets Automation
Chang points to other industries for the benchmark of how automation can work. Finance, airlines, theme parks all provide examples of industries which have conquered automation in a way healthcare has yet to achieve.
“For some reason healthcare is not as automated and it’s highly fragmented. Unfortunately, that’s causing increased costs and general unhappiness for the healthcare consumer,” Chang said.
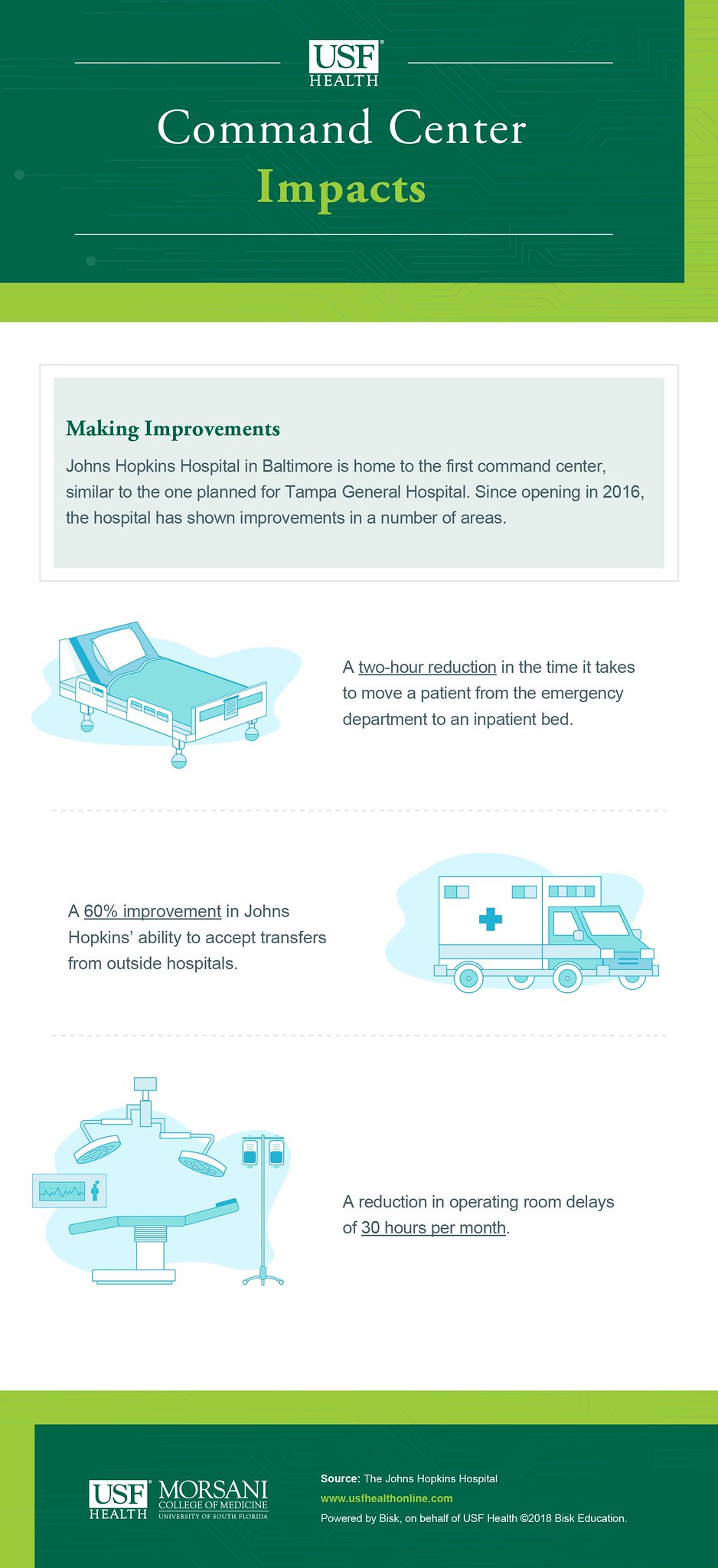
The Command Center changes that. Inside Johns Hopkins Hospital’s Judy Weitz Capacity Command Center, banks of computer monitors keep two dozen staff members representing various departments abreast of the entire facility.
The Command Center alerts and enables them to address issues as they arise which can include, according to the hospital’s website, “when there is an influx of patients coming into the hospital, which hospital units need additional staff members, the status of how many patients are being treated, the need for and availability of beds across the hospital, the highest-priority admissions and discharges, and other information essential for ensuring high-quality patient care.”

During a typical afternoon, the system receives about 500 messages per minute from 14 different Johns Hopkins IT systems generating real-time data to trigger action throughout the hospital, according to the site.
Like Johns Hopkins’ center, TGH’s will be powered by GE’s Wall of Analytics which includes electronic tiles that gather data from sources around the facility such as admissions software, operating room scheduling applications and electronic health records (EHRs). The tiles themselves can be viewed individually on computers or mobile devices outside the center. The wall can be reconfigured to focus on a single event if necessary.
From Operational to Clinical
The Command Centers primarily have been focused on what Chang calls operational tasks — “transport times, environmental services, communication, even putting in diet orders, making sure patients are getting the right meals, coordinating equipment and services and scheduling, that’s all strictly operational.”
While the centers have proved successful at reducing wait times for hospital beds and ambulances, Chang wants to see them take on more complex tasks.
“I hope that in the near future we transition from an operational basis to more of a clinical one,” Chang said. “Can you use artificial intelligence and predictive analytics to figure out if there are trends with vitals, meds, labs and clinical documentation that may tell us a patient is heading in a bad direction, versus waiting for a provider or nurse to put together the clues to figure out what’s going on?”
This will occur through a process of developing clinical pathways for early identification of serious disorders and diseases that can occur in hospitals, such as sepsis, a severe bloodstream infection.
“You look at all these different pathways and you ask, ‘Can I not only identify them earlier, but can I start to notify my providers and then initiate treatments earlier?’” Chang said. “That only comes from that really strong, predictive analytic modeling, and that comes from looking at what’s happened to patients in the past, when they’ve developed deteriorations and tying that back to the data that’s coming in live from the patient. That’s a huge benefit.”
GE’s Terry believes that day will be here soon.
“AI is also very good at predicting things,” Terry said. “We can start to find the patterns and based on what’s happening now we can see a problem coming tomorrow, whether that’s a canceled surgery or a canceled imaging procedure or a patient at risk, we can predict many of those things with AI.”
According to Terry, TGH is producing a megabyte of data every second. Where patients are going, what they are doing, tests and procedures that are ordered, what physicians they see, what were the results: all of it is information that the command center can track.
“Caregivers are already putting that data to work but there’s so much more that can be done,” Terry said. “That’s where artificial intelligence comes in, looking at data from the EMR, from machines, from other software centers, from devices.”
In the end, it’s the combination of human and artificial intelligence that gives the Command Center its full potential.
“Artificial intelligence combines with human intelligence to spot the needle in a haystack — to find the patient at risk, to suggest the thing we can do now that will prevent the delay tomorrow,” Terry said. “That combination of a department that is thinking about helping patients and is looking across the enterprise with the artificial intelligence to focus them – that’s what a command center is.”



